 <
<
 >
>

Chapter 2:
Escharotics:
500 Years of Suppression
 "The touchstone of true science is power of
performance, for it is a truism that what can,
also will, and thus attains to real existence."
"The touchstone of true science is power of
performance, for it is a truism that what can,
also will, and thus attains to real existence."
Dr. Rudolf Virchow
(1821-1902)
 "The universities do not teach all things ... so
a doctor must seek out old wives, gypsies, sorcerers,
wandering tribes, old robbers, and such outlaws
and take lessons from them. A doctor must be
a traveller . . . Knowledge is experience."
"The universities do not teach all things ... so
a doctor must seek out old wives, gypsies, sorcerers,
wandering tribes, old robbers, and such outlaws
and take lessons from them. A doctor must be
a traveller . . . Knowledge is experience."
Paracelsus
1
(1493-1541)
 "Any treatment of disease that claims to be in
advance of what is known to the profession however
clearly on scientific principles or uniformly
commended by its power to heal, is sure to meet
with opposition. In the treatment of cancer that is
the more to be expected inasmuch as cancer has been
the opprobrium of the profession. By physicians,
the world over, it has for the most part been regarded as incurable.
If this is not so, why the conviction
universally pervading the public mind that
all ordinary means to arrest it are impotent?"
"Any treatment of disease that claims to be in
advance of what is known to the profession however
clearly on scientific principles or uniformly
commended by its power to heal, is sure to meet
with opposition. In the treatment of cancer that is
the more to be expected inasmuch as cancer has been
the opprobrium of the profession. By physicians,
the world over, it has for the most part been regarded as incurable.
If this is not so, why the conviction
universally pervading the public mind that
all ordinary means to arrest it are impotent?"
T.T. Blake, M.D.
2
Cancers Cured Without
the Use of the Knife (1858)
 "A physician once told me that nothing arouses
so much bitter enmity and heated arguments among
his colleagues, as the subject of cancer. This
may be due to the guilty recollections of cancer
victims expiring who might have been saved;
or of the memories of patients pronounced
hopelessly ill who recovered under the treatment
of a 'quack,' or who miraculously lived without
further treatment. Possibly these guilt reactions
and the remorse over exhausting the money of
patients and their relatives in futile cancer
treatments, account for some of these psychological
manifestations which are expressed in hostility
and attack."
"A physician once told me that nothing arouses
so much bitter enmity and heated arguments among
his colleagues, as the subject of cancer. This
may be due to the guilty recollections of cancer
victims expiring who might have been saved;
or of the memories of patients pronounced
hopelessly ill who recovered under the treatment
of a 'quack,' or who miraculously lived without
further treatment. Possibly these guilt reactions
and the remorse over exhausting the money of
patients and their relatives in futile cancer
treatments, account for some of these psychological
manifestations which are expressed in hostility
and attack."
Nat Morris
3
(written in 1958)
 "I die by the help of too many physicians."
"I die by the help of too many physicians."
Alexander the Great
3b
On his deathbed, 323 B.C.
 "Civilization originates in conquest abroad and
repression at home."
"Civilization originates in conquest abroad and
repression at home."
Stanley Diamond
4
In Search of the Primitive:
A Critique of Civilization
 t is my position that
for the entirety of recorded history in
Western culture, but most particularly on account of Greek and
Roman influences from about the fifth century, B.C., to the present,
the suppression of simple, effective medical remedies in
favor of more complex systems, methods, products, and protocols,
has been embedded into the very fabric of the prevailing
medical establishment. We'll examine the various political, economic,
and religious constructs -- my version of "cultural
infrastructure" -- necessary to sustain this system of
suppression in an upcoming section. For now, it is only
important to establish and define the "suppression pattern"
and apply it to escharotics, as we discussed in the first chapter,
so as to first finish my initial chronology.
 An example of a famous medical pioneer who actually USED
escharotics, is well documented in his success in treating cancer,
was well-known to have been a victim of jealousy among his less
competent colleagues (which included nearly everyone save himself),
and was finally disposed of as a means of terminating their frightful
embarrassment, should serve the present purpose.
 He lived in the 16th century.

 Most physicians of antiquity acquired their reputation
not because they were great theoreticians, but because they
were able to cure patients who found little relief elsewhere.
The proof was in the pudding. Good doctors cure their patients,
and grateful acknowledgement through payment is the natural
consequence. (Today it's the reverse. Getting paid is primary.
The cure is an after-thought. This is poignant reality that
hits anyone who has ever visited the ER section of a
modern American hospital.)
 A master of empirical eclecticism in the medical arts,
Paracelsus gave credence to neither academic credentials nor social
standing. He understood the dangers inherent in ideological
rigidity and was the very antithesis of monoculturalism
in medical approach, in all its diverse theoretical and applied
facets that are as much an infection in medicine today as it
was back in the days of Galen.
 Paracelsus is reviled for his association with mysticism,
astrology, and alchemy by contemporary historians -- indeed
he found ways to harness them all in his practice -- and yet
his critics must begrudgingly note his unusual successes.
Centuries before Mesmer, Paracelsus understood and employed
the principles of suggestion; centuries before Freud, he
understood mind/body connection; centuries before Antonio Meucci
5
or R. Raymond Rife,
6,7
he utilized electromagnetic therapy; he discovered
hydrogen, nitrogen; coined the term "alcohol" (from the Arabic)
8,
and identified zinc. He composed his own pharmacoepia and
achieved clinical success that few physicians today can match --
all at a time when medical specialization, as we know it, was
non-existent.
 Gotthold Ephraim Lessing (1729-1781),
one of the most influential figures of the Enlightenment, said
of him, "Those who imagine that the medicine of Paracelsus is
a system of superstitions which we have fortunately outgrown,
will, if they once learn to know its principles, be surprised
to find that it is based on a superior kind of knowledge
which we have not yet attained, but into which we may hope
to grow."
9.
His knowledge of subtle energies that act
upon the living organism mimic principles that only now are
beginning to migrate from our recent discoveries in quantum
physics into the stodgy crevices of our biological sciences.
Paracelsus is widely credited with not only being the "father of
modern medicine" -- in part because of his expansive and
radical departure from the apothecary practices of
his time -- but the father of lesser known or respected
practices and disciplines, including iatrochemistry
and balneology.
10.
Viewing the breadth of his work and
the endurance of so many of his ideas (not to mention a
universe of thought that did not endure -- perhaps because
we have not the sufficient collective consciousness to
comprehend them), it does not seem hyperbolic to say
that he was "the precursor of chemical pharmacology and therapeutics,
and the most original medical thinker of the 16th century."
11
 In a facet
of personality that appears common among those
who rise too far above the mean intelligence of their medical
peers, Paracelsus appeared to have little by way of humility.
While lecturing at the University of Basel, he is reported to
have said that the soft down on the back of his neck knew more
about the practice of medicine than all the professors of Basel
put together
12.
A celebratory book burning of works by
Galen and Avicenna, pillars of 16th century medical thought,
which Paracelsus orchestrated in the spirit of religious
leader and fellow German reformer, Martin Luther (1483-1546),
was the last straw for many. It wasn't enough that he could cure
illnesses that no one else could, he made a point to rub his
colleagues collective face in it. On one occasion Paracelsus
offered to cure any patient deemed incurable. Fully prepared
to disgrace this wild braggart, his colleagues presented him
with fifteen advanced cases of leprosy. (One can only imagine
that since his enemies got to do the choosing, these were no
mean challenges. No doubt with advanced cachexia and one foot
already in the grave).
 He cured nine out of the fifteen.
13.
 The escharotic
formula that Paracelsus used was as simple
and direct as the rest of this practice. Instead of zinc
chloride as a caustic halide, Paracelsus used "sal ammoniac"
(ammonium chloride), along with fuligo (wood soot), and
orpiment (arsenic sulfide).
14.
According to records of
the time, it worked. (Interestingly, Paracelsus
employed his own "arsenic paste" nearly 400 years before
Nobel Prize-winner, Paul Ehrlich, created his own celebrated
version to treat syphilis in the early 1900's.
15.
Variations
in the 1800's had already been used by allopaths to treat
skin cancer).
16
 Paracelsus
had a separate formula that was less
"intense," which he used to treat skin cancers,
jaundice, and some wounds. We don't know the exact
method of preparation, but it used "litharge" (lead
monoxide) as the caustic agent.
17
 As one
might expect, Paracelsus' reviling of tradition
would eventually cost him his life, as he was unceremoniously
pushed off a cliff by hired assassins "in the employ of
the medical fraternity," according to supporters.
18 Though
even a most orthodox review of Paracelsus'
contribution to modern medicine cannot diminish his stature,
the allopathic version of his end, as with most dissenters,
has him in a most unflattering exit off stage -- namely,
a bar room brawl
19
Or victim of a midlife stroke.
20
The reputation of more recent dissenters who produced
miraculous results has faired no better -- even to the
point of altering a death certificate.
21
 Paracelsus
was my illustrative choice here not only because
he was a medical luminary nonpareil, but because the elements of
suppression are most vivid in his life and work -- such as I have
most scantily summated here.
 Central to
Paracelsus' work was the use of natural plants
and mineral compounds, and what we might regard as the rudiments
of modern chemistry. He didn't abandon Galenian concepts of
herbal medicine, but his understanding was deeper, richer, and
more holistic -- turning empirical, "evidence-based" medical herbalism into a
kind of subset of a much larger universe of thought and practice.
 There are
hundreds of botanical extracts, the knowledge of
which come to us from indigenous sources worldwide, which have shown
to have anti-cancer properties. Dr. Jonathan Hartwell, one of the
founders of the National Cancer Institute, spent most of his
adult life categorizing them, leaving behind a reference that
would become a classic in the field of phytopharmacology
and ethnobotany.
22
(Later I would write an article, in
tributary devotion to Hartwell's influence on my own work.)
23
 But
escharotics are not just botanicals. They employ,
by definition, a lightly caustic compound, with one or more
botanical ingredients. Caustics usually involve the use of
a metal salt, often a halogen combined with a metal (halide),
such as zinc chloride or potassium iodide.
24
(Though in the case of one famous physician,
the contribution of the dissociated
potassium was considered paramount.)
25
 Another anhydrous chloride,
"butter of antimony" (antimony trichloride) fits into this
category. Many dermatologists are aware that along with
zinc chloride, butter of antimony was one of the
ingredients in a number of early escharotics of the
1900's.
26
But its use goes back even to Paracelsus
in the 1500's -- though it appears he used it for other
maladies.
27
 I always
stuck with zinc chloride in my escharotic
work, and if you spend a couple hundred hours (as I have)
going through patent records to uncover what caustic
previous researchers have used, zinc chloride is, by
far, the caustic of choice. Familiarity with its useful
properties is not new. Anthropologists found traces
of man-made zinc chloride in the Pyramid at Giza,
produced at LEAST 2,500 years ago -- (though one
researcher attributes its use to the generation
of power and not medicine.)
28
 Zinc chloride,
though now reviled by allopaths in
an attempt to smear alternative practitioners, was one
of just three ingredients in the initial Mohs surgical
paste that is now central to a standard dermatological
procedure approved through the West. The three ingredients
that Mohs used in his formula and taught were: zinc
chloride, bloodroot, and stibnite (antimony sulfide,
another Paracelsus favorite)
29 ,
and can be found
in Mohs own original work.
30 .
Ironically, the
AMA, FDA and other pillars of orthodox medicine exerted
enormous effort to put Harry S. Hoxsey out of business
(and they succeeded)
31,
and yet Hoxsey's formula
was almost identical to Mohs. The difference? Mohs
called the topical a "fixative," and he artificially
and unnecessarily inserted the act of surgery as a
necessary part of the process.
32
 Hypocrisy
and suppression have appeared together
as cousins throughout the history of organized medicine,
as we'll see time and again.
 (By the way,
American physicians are
now taught that zinc chloride was eliminated from the
Mohs paste as an ingredient because it is caustic
to healthy skin tissue. There is no nice way to say this:
it's a patent lie. I myself have worked with "butter of zinc"
bases that were over 60% pure zinc chloride and had the
thick, syrupy mess dripping from my fingers down to
my elbow for the better part of an hour. Upon removal
with running tap water there was only slight irritation
to the skin on my forearm. I have done this not less
than fifty times in a twelve year period -- 1991 to 2003.)
 The
suppression of effective, inexpensive, natural
methods of healing has a history in the U.S. that is
more extensive and egregious than any place on earth, in any time
period on earth. I didn't realize just how true this was
until I compared various escharotic patent filings in the
U.S., with court filings on Hoxsey, Rife, and others, and
then compared this with published work on the subject.
 In late 1857
and 1858,
three separate medical doctors surfaced
in the U.S. and England with reports of a cancer cure
that worked with amazing success.
33
 The first was Dr. J. Weldon Fell.
 A man
of no plebeian upbringing, Fell was
born to an old and distinguished American family with
a long lineage of famous physicians and professional men,
Fell was one of the original founders of the New York
Academy of Medicine and a faculty member of the University
of New York -- and as cancer writer Nat Morris noted,
his was "one of the most interesting (stories) in the history
of cancer."
34-36
 According
to Morris, "... a sinister cloud enveloped
his career because of his cancer practice and in the
prime of his life, he emigrated to London to start
anew. There he engaged again in the practice of cancer
under very auspicious circumstances for he was singularly
prosperous and lived very lavishly."
 His departure
from New York was shrouded in mystery,
but it fits a recurring pattern for physicians whose
cancer practices rise too far in success above their
peers. Prior to leaving, Fell attempted to resign
from the New York Academy of Medicine, but his resignation
was refused. It appears his association with a
"cancer quack," a certain Gilbert of New York City,
had caused colleagues great animosity. His resignation
was postponed in the hope of "pinning a charge of
quackery upon him so he could be ignominiously
ejected from the academy."
 Fell's
subsequent success in London provides
evidence as to the cause of his mistreatment in New
York, as does the sizeable fortune, earned while
servicing a grateful, sizeable base of patients
in the U.S., which he took with him to England.
He wrote a friend of renting a castle for $100
per week, a kingly sum at that time.
 In the
fine tradition of Paracelsus, Fell was
also a man lacking in humility. A mere guest in
his new host country, he derided English
surgeons for "operating and amputating without
any justification whatsoever and said that limbs
were cut off merely to satisfy the vanity or
sadism of surgeons. He charged that practices
were tolerated in England that would never be
permitted in the United States and of all the
physicians he had met in London, there were only
two whom he would trust to treat himself or
his family."
37
 Remarkably,
excepting these sharp comments
on the surgical practices of his contemporaries,
Fell remained on good terms with his fellow
English practitioners, and although little is known
of the final years of his life, the record shows
that he never again fell into disrepute -- alleged
or otherwise, professional or public -- again.
 Dr. Fell
published a text on cancer, the
content of which is the basis for his inclusion
in the present work.
37b
 To the best knowledge of this
author (and I would be delighted to hear from anyone
who would refute my assertion) Fell was the first one
to publish an escharotic as it has come to be most
popularly used in the West -- namely, the use of zinc
chloride as the caustic of choice, along with a
cancerolytic (cancer-fighting) medical herb.
The use of zinc chloride as a superior, though
mildly, caustic (it has a pH of 5.0), is reflective
of the experimentation that took place over the
preceding centuries. Caustics known to have
been used, then and prior, in orthodox practice
included "nitrate of silver, quicklime, sulphate
of copper (sometimes used with borax), sulphuric
acid (oil of vitriol) mixed with saffron, and
permanganate of pottasa. Alkaline caustics
such as sulphate of zinc were also in vogue."
38
Dr. Fell dismissed them all, so he must have
known of their shortcomings, as did his contemporary
and fellow user of escharotic preparations,
Dr. John Pattison (see below).
 Fell's
publication itself places him 20 years
prior to the filing of U.S. Patent No. 209,311, and just
four years after A. Hunton's 1855 treatise, "On some of the
medical virtues of indigenous vegetables grown
in the United States." We are also told by Hunton
that the manner in which the medical secrets concerning
bloodroot were obtained from an Indian doctor were less
than honorable.
39
(None of which compares, of course,
with the rapacious pilferage of indigenous Americans'
land and most of their very lives.)
40
 Even
apart from Fell's open admission that the
central role of bloodroot in his medical product came
from native savages,
41
there is the issue of its
use in American folk medicine long before that,
specifically, its widespread use in Pennsylvania,
documented as early as 1811.
42
Moreover, since
bloodroot is native to the North American continent,
its appearance in Russia infers that it may have been
exported there.
43
Internal studies by the
National Cancer Institute, which have themselves
been suppressed, show even wider use in recent
times.
44
 But again,
it is Fell that publicly announces
the advancement of an escharotic by adding bloodroot
to zinc chloride. Of greater importance is the
final report which the board of directors of Middlesex
Hospital allow him to publish concerning the results
on 25 cancer patients, substantiating his claims
that his treatment was far more successful than
anything then available "and justified abandoning
surgery for relief of cancer."
45
 In their
official communication, the board
made the following cautious endorsements of the Fell
cancer treatment:
- It was safe and conformed to surgical principles
- It could be employed on both operable and
inoperable cancers.
- It obviated removals of the entire breast
and could be confined to enucleation of
tumors only.
- It spared patients the hazards of surgery,
including hemorrhage and constitutional
affections.
- Enucleation was followed by healthy granulation
and cicatrizing surface (scarring over).
46
 Despite
its apparent growing acceptance by
the orthodox medical community in London, a sea change
that should have brought about the elimination of
radically invasive cancer procedures, the remedy
somehow fell into disuse. Only sporadic, historical
references can be found to its use, which demonstrate
that conscientious physicians would discover and bring
the practice back, only to see it furloughed by medical
authorities. One such instance is the use of a
zinc chloride compound at St. Bartholomew Hospital
in London -- to treat breast cancers, no less. (Our
knowledge of it survives because two such cases
can be found in the hospital's "Pathological Museum.")
47
 For now
it's important to know that Fell was
not alone in his discovery -- even in his own time.
 At At
about the same time that Fell was making
headway at Middlesex Hospital, Dr. John Pattison,
also an expat from New York City living in London,
was also preaching the same message with what appears to
be the same formula. Pattison, like Fell, abhorred the
surgical treatment of cancer as a fraud upon the public.
In 1858, Pattison, too, published his own work,
a pamphlet, which provided not only the exact
formula, but a precise description of its use.
His ingredients? Zinc chloride, goldenseal
(hydrastis canadenisa), flour and water. (This
author, having experimented with variations of
both formulas over many years, can attest that
the end result of either Fell or Pattison's
formula would be almost indistinguishable topically.)
To further punctuate his point, Pattison expanded his
pamphlet to a book in 1866, entitled "Cancer:
Its nature and successful and comparatively painless
treatment without the usual operation with the knife."
48
 Neither
Fell nor Pattison were obsessed with
the elimination of more invasive methods of cancer
treatment without sound reasoning. As early as
1844, a survey was compiled by Dr. Leroy-d Etoilles
and published by the French Academy of Science.
To this day this report on cancer survival is
probably the most extensive ever released.
It was based on results supplied by 174 physicians
on 2,781 cases, followed "in some instances
for over thirty years."
49
The short version:
patients are better off, in most cases, doing
nothing at all than going with surgery. Today,
despite modern improvements in techniques and
equipment, "the dominance of surgery in the
treatment of cancer despite these ominous
observations has been maintained by studiously
ignoring and suppressing adverse information
by the powers that be."
50
The continued
practice of unnecessary surgery for financial
gain is a contributing factor in "death by
doctoring" as the third leading cause of death
in the U.S. -- so says a study that miraculously
managed to find its way into the pages of the
Journal of the American Medical Association as
recently as 2000 -- though it was largely
ignored by the mass media.
51
 Pattison
was not singular in his approach.
(No physician worth his salt is.)
He indicated the role of diet, reflecting the
etiological role of nutrition that was a century
ahead of its time. Despite the later dating
of his publication, Pattison's involvement with
the very same Middlesex Hospital that brought
fame to Dr. Fell is quite insightful. As it
turns out, Pattison's work in London came
BEFORE that of Fell. In 1852 Pattison offered to demonstrate
his method to the directors of Middlesex Hospital
and even to work without pay. An initial
agreement was worked out where Pattison would
work with twenty cases and would disclose his
methods, permitting disclosure of his methods
and criticism of results.
 The
directors reneged.
52
 A subsequent
request in 1854 was also sent begging. Pattison
continued to work in London, where he built a
successful practice that was wide and extensive.
Nonetheless, Pattison was labelled a "cancer
curer" and "quack" by his medical colleagues.
His name was deliberately omitted year after
year in the semiofficial directory of physicians,
an act of mean-spiritedness that was only changed
by an act of Parliament.
 In
comparing the life work of Fell and Pattison,
one point becomes most instructive. Their formulas
and protocols were, from a functional point of view,
nearly identical. So why did the medical community
accept one with open arms and slander the other as
a quack? This is one of many anomalies in the cancer
establishment that defies logical explanation.
Why did U.S. Federal authorities come after me because
my Cansema, whose active principles were in the
zinc chloride and chapparal, both of which appear or
have appeared in approved cancer related products
(in Mohs' surgical paste and Actinex (NDGA))?
Why was I made to plead to selling "an unapproved drug"?
Is it because NDGA is okay if it's made in a laboratory,
but not okay if it comes from chapparal, the very
plant from which the discovery was made -- a plant
with an extensive ethnobotanical history of use
for medical purposes?
53-56
 You
find these and so many other "non sequitors"
and "profit over logic" contradictions throughout the
medical industry.
 The
third and last practitioner / specimen
from 1858 is also instructive. T.T. Blake, M.D.,
published "Cancers Cured without the Use of the
Knife." Unlike Fell and Pattison, Blake would not
reveal what his formula was. Nonetheless, the
description he gives of the process follows so closely
those of all other escharotics, and taking into
account the uncanny origin of Pattison and Fell
in New York during the very same time period,
I would agree with Nat Morris' interpretation that
it was most probably an escharotic formulation
that was close to theirs.
57

The Extraordinary Case of Perry Nichols, M.D.:
A 20th Century Story of a Cancer Clinic That
Cured Cancer Using Escharotics for 60 Years:
1896-1956
 By the end of the 20th century,
the successful use of escharotics for the better part of a half century
had become so widespread that various clinics and institutions began
to specialize in it. None that I know of is more noteworthy than
the case of the Dr. Nichols Sanatorium of Savannah, Missouri.
This institution cured more than 70,000 patients of cancer between
1896 and 1956 -- many of whom would have been regarded as untreatable
by even today's best oncologists.
58
 As I write this addition to Chapter 2
(Apr., 2017), I reflect on the various references to the Sanatorium that
I have received over the past 25 years. (Nichols Sanatorium in Savannah, Missouri,
would be the home of Nichols' operation for its last 44 years.) I would have included more
references to Perry when I wrote the first draft of Meditopia in 2004,
but I demurred for lack of material.
 Early last year I contacted the
Andrew County Museum
and Historical Society in Savannah and was surprised to find a wealth of
material concerning the Sanatorium, which closed in 1956 -- the year I was born.

 The specifics of the Sanatorium beginnings
are simple enough: Its founder, Perry Nichols, was born in Benton County, Iowa,
on March 20, 1863, worked with a clinic specializing in escharotic medicine in 1895,
started up his own clinic in 1896 (hiring a physician to work with the patients),
graduated from medical school himself in 1901, and later established a 200-bed hospital
in Savannah, Missouri.
59
He incorporated the Sanatorium in June, 1914, however, by this time he had already
developed a widespread reputation of
successfully curing cancer using his own techniques. "It was only after many years
of research and diligent study that he discovered a safe and sane cure for the
malignant disease of cancer without the use of the surgeon's knife and the miraculous
cures that he has performed entitle him to the gratitude of thousands of patients
and should give him eminent standing among the benefactors to mankind. His institution
is modern in every way, with skilled medical practitioners and corps of trained nurses,
and the location of the building is in a section where may be found every requirement
of health. Although Doctor Nichols has built up this enormous business in but a few years
and has comfortable accommodations for many patients, coming from every section of the country,
at the present writing (1915) he is comtemplating further extension, which means still further
humanitarian usefulness."
60

 Above: The phenomenal success of the Nichols clinic is a cautionary
tale about the frivolity of "acceptable" historical texts . . . or as the French philosopher, Voltaire,
so succinctly put it: "The history of humanity is a Mississippi of lies." In this case, I would add "omissions."
For the omission of the successful history of the Nichols Sanatorium from any other meaningful text on the history
of cancer in the U.S. leaves a permanent black hole of deceit, intended to hide the ease with which
cancer was so easily and inexpensively treated more than a century ago. The photo above is a photograph
of the Nichols' staff, circa 1925. Above: The phenomenal success of the Nichols clinic is a cautionary
tale about the frivolity of "acceptable" historical texts . . . or as the French philosopher, Voltaire,
so succinctly put it: "The history of humanity is a Mississippi of lies." In this case, I would add "omissions."
For the omission of the successful history of the Nichols Sanatorium from any other meaningful text on the history
of cancer in the U.S. leaves a permanent black hole of deceit, intended to hide the ease with which
cancer was so easily and inexpensively treated more than a century ago. The photo above is a photograph
of the Nichols' staff, circa 1925.
 Those who might suggest that the success of the Nichols Sanatorium
would be based on some kind of personality cult originating with its founder should know that the involvement
of the founder was short-lived. Dr. Perry Nichols, a tireless workaholic, died of a heart attack on August 29, 1925
at the age of 62.
61
Thereafter, his daughter, Mrs. Helen Nichols, took over the management of the Sanatorium, in accordance
with his will.
62

 The successful work of the Sanatorium was represented
in its annual "yearbooks," that the institution produced, year after year. (The photo at right
shows seven volumes that I have managed to collect over the years.) Additionally, the Sanatorium
managed to put out an enormous amount of catalogs and postcards. The voluminous amount of
printed materials that the Sanatorium produced was, in part, an effort to overcome the conventional
medical propaganda about cancer treatment -- disinformation that has changed little over the
past century. As the 1929 yearbook stated in its introduction, "Were it not for the fact that a
great many people are constantly making declarations that cancer cannot be cured; were it not for the
fact that the majority of physicians and surgeons are advocating, as you will see published in popular
magazines, that 'the knife, radium, and X-ray' are the only remedies, the publication of this book,
which contains the proof that such declarations are false, would not be a necessity. We submit this
book, with the facts as quoted, and a list of thousands of references, for your consideration.
These are cured patients, and now living . . ." At the end of 1929, at the beginning of the
Great Depression, the Sanatorium experienced its greatest year ever -- mailing out 13,000 catalogues
to the public.
63
 Throughout the Depression, the Sanatorium continued to prosper.
In 1942, at the start of
America's involvement in World War II, the news of one mailing alone made it to the local paper:
a mailout weighing 52,000 pounds. Four years later, in 1946, the Sanatorium produced a catalogue with
over 350 pages and an "annual list of cured patients containing almost ten thousand names and addresses
of recently cured patients." Given that the Sanatorium only reproduced the names and address of cured
patients who formally gave their permission to have their personal contact information reproduced, one
can only wonder what the Sanatorium's true impact was.
64

 Above: Over the life of the Sanatorium, untold thousands of its
postcards were sold to the public and distributed through U.S. Postal. I bought the one above last
year (2016) from CardCow. It's addressed to:
"Mrs. J. Winsler (of) Abilene, Kansas." There is no other address information because at that time,
nothing else was necessary for letters sent to rural America. The postmark says May 13, 1920,
and the writing on the back of the card is typical. "Have received a letter from my sister, Mella,
telling me of your poor health. We have a neighbor who was cured of cancer at the institution
advertised on this card, 6 or 7 years ago. He says they are fine. I certainly hope you do not
have it (cancer) at all. We are all well. Boys are doing fine. They are working their way through
college. Hope your boys and the family are well." Above: Over the life of the Sanatorium, untold thousands of its
postcards were sold to the public and distributed through U.S. Postal. I bought the one above last
year (2016) from CardCow. It's addressed to:
"Mrs. J. Winsler (of) Abilene, Kansas." There is no other address information because at that time,
nothing else was necessary for letters sent to rural America. The postmark says May 13, 1920,
and the writing on the back of the card is typical. "Have received a letter from my sister, Mella,
telling me of your poor health. We have a neighbor who was cured of cancer at the institution
advertised on this card, 6 or 7 years ago. He says they are fine. I certainly hope you do not
have it (cancer) at all. We are all well. Boys are doing fine. They are working their way through
college. Hope your boys and the family are well."
 Interestingly, I am not the only one who has found the
Nichols Sanatorium story fascinating. His story
has been summarized on
Whale.to and in 2004, Dermatology Times ran a story by a Andrew Bowser, M.D.
about a dermatologist, Dr. Gary A. Dyer of Joseph, MO (just 13 miles from Savannah)
who claims that he spent two years "piecing together a history of Nichols, interviewing
nurses who worked in his institution, and scouring medical archives and local historical records.
(I have) monitored eBay and Internet booksellers for surviving copies of yearbooks Nichols wrote touting
his methods, patient testimonies, and cure rates . . . "
65
 Dyer traced Nichols' knowledge of the technique upon which
he would later build his empire, to a visit to an Iowa clinic in 1895, where -- at the age of 32 --
learned about treating cancers escharotically from two doctors who ran the "Cherokee Sanatorium."
(By that time, many medical doctors, who at that time belonged to a fairly close-knot fraternity
were privately familiar with escharotics -- many from the work of the men whose work is discussed
above and others from the patent work that had already been filed in Washington.) After spending
time working at the Cherokee Sanatorium, Nichols set to work on his own escharotic formula and
then opened his own clinic in November, 1896.
66
 As to the burning question --
what exactly was in Nichols' formula?" -- Dyers found a 1933 article in the
Journal of the American Medical Association which revealed (probably through surreptitious
acquisition) the results of its analysis: zinc chloride (ZnCl2) and butter of antimony (antimony
trichloride or SbCl3). ). Dyers goes on to note: "Interestingly, in a skin pathology and treatment textbook
published in 1895, Kaposi described a 'modified Landolfi's Paste' consisting of zinc chloride and
butter of antimony." Then Dyers goes on to note (as I did in the previous chapter) that this is close
to the initial paste used in Moh's surgery, consisting of zinc chloride and bloodroot.
67
 But the small formulary difference --- and when you understand
the effects of these different combinations, you realize they are quite close --- was not the only thing
separating Nichols and Moh. Moh "championed biopsy," a big industry money-maker, even though
biopsies are inherently metastatic,
thus guaranteeing future business. Nichols, on the other hand, understood, as did Hippocrates 2,300 years
before him, that cutting into cancer aggravated and stimulated malignant growth.
 Dyers ends his article by saying that if Nichols had gone a more
conventional route -- (using an on-staff pathologist) -- he could have "made the discovery" that Moh's
made later and been much more successful.
 This is nonsense. It's nonsense because what Moh did was co-opt
an existing medical modality and attempt to make it more profitable for the profession. Dyers admits
that from July, 1931 to June, 1948, the Nichols Sanatorium -- which treated several thousand patients per
year -- was only averaging about 70 surgeries annually. If you treat 7,000 patients and subject 70 of them
to surgery, that's 1%. That's a little bit less than the Moh's procedure, which calls for surgery 100%
of the time. Which approach is likely to be more profitable?
 One thing I wasn't able to determine from any of the materials
I read was the exact reason the Nichols Sanatorium closed in 1956. The Sisters of St. Francis,
who moved in shortly thereafter to set up a nursing home at the hospital, were hardly the reason for
the closure. What we do know is that by 1956, the public practice of escharotic medicine in the
United States was clearly under attack. Given the public airing of Harry Hoxsey's travails, it is
difficult to imagine anybody in the administration of Nichols' Sanatorium not knowing that the
American Medical Association, Food & Drug Administration, and other minions of the Medical
Industrial Complex were -- even then -- committed on putting Nichols' Sanatorium, and small organizations
like it, out of business . . . taking them to court, fining them to death, hopefully imprisoning
those in charge, etc.
 It is thus most logical to surmise that a decision was made
to close Nichols Sanatorium, concluding 60-year of uninterrupted and successful medical practice,
in the most graceful and non-combative way possible.
 And -- as it turns out -- that's exactly what they did.
 [ See Nichols Sanatorium Pictorial
in the right column for more.] [ See Nichols Sanatorium Pictorial
in the right column for more.]
 I feel
quite certain that these historical
cases represent mere shadows in the long list of
practitioners who have used escharotic preparations.
They were hugely successful and their clinical
reports were most positive. So, why did escharotics
fall into disuse?
 Is it
possible that the answers can be found
in the
" Ten Conditions"
discussed in Chapter One? Is
there a logical explanation that would refute them?
Even in the medical records of antiquity we find
evidence of the ubiquitous practice of suppression
towards those therapeutic practices that would
pose the greatest threat to organized medicine.
 Long
before the escharotic publications
and pronouncements of 1858 -- indeed, long before
the miraculous cures of Parcelsus himself, the
truth was evident to all who would investigate
without vested interest. Paracelsus himself,
in attempting to promote his accomplishments
chose a namesake that would not refute the
soundness of his escharotic protocols.
"Paracelsus" is Latin for "above Celsus" --
so who would Celsus have been that Paracelsus
chose him as a point of lofty comparison?
Why not "Paragalen"?
 Shortly
after the invention of printing
press around 1450 by Johann Gutenberg, one of
the first medical works to be published was
"De medicina," by Aulus Cornelius Celsus, the
first century Roman physician and medical writer.
68
Its initial publishing in 1478, just fifteen years
before Paracelsus' own birth, would lead to wide
acceptance in the orthodox medical community. Divided
into three parts, according to the type of treatment
that various diseases demanded -- dietetic, pharmaceutical,
and surgical -- Celsus' work laid the
foundation for many of the components of the modern
medical paradigm in ways even more fundamental
than those of Paracelsus. Even Celsus believed
that "caustics should be tried before knife or
cautery."
69
Before him, "caustics" were used by
early Arab and Roman physicians.
70
Viewed from
a historical perspective this long, is it really
possible that a truly effective way of curing
cancer could so easily be suppressed?
 In time,
you'll be able to answer this question
for yourself, but since I myself sold my own
escharotic preparations to untold thousands of
practitioners and end users worldwide from 1990
to 2003, perhaps I should finish telling you my
own story.

- The New Encyclopaedia Britannica, 15th Edition, 1986,
Vol. 9 (Micropaedia), "Paracelsus," p. 134.

- T.T. Blake published
Cancers Cured Without
the Use of the Knife in 1858. The passage cited from the book is taken from: Nat Morris,
The Cancer Blackout,
Regent House, Los Angeles, Calif. (USA), 1977 (Fifth edition), p. 28.

- Nat Morris, The
Cancer Blackout, Regent House, Los Angeles, Calif. (USA),
1977 (Fifth edition), p. 156.
 ---- 3b --- Alexander the
Great quote taken from: George Crile, Jr., M.D.,
Cancer and Common Sense,
Viking Press, New York, 1955. Chapter VI, "The Hidden Cost of Cure," p. 51.
---- 3b --- Alexander the
Great quote taken from: George Crile, Jr., M.D.,
Cancer and Common Sense,
Viking Press, New York, 1955. Chapter VI, "The Hidden Cost of Cure," p. 51.

- Stanley Diamond,
In Search of the Primitive: A Critique
of Civilization, as quoted by Jensen, p. 189.

- Gerry Vassilatos,
Lost Science, Adventures Unlimited Press,
Kempton, Illinois (USA), 1999, "Chapter 2: Hearing Through Wires:
Antonio Meucci," p. 56-75.

- Ibid., "Ultra Microscopes and Cure Rays: R. Raymond Rife,"
p. 137-168.

- Barry Lynes, The
Cancer Cure That Worked!, Marcus Books, Ontario, Canada, 1987.
- http://www.wordiq.com/definition/Paracelsus

- http://reference.allrefer.com/encyclopedia/L/LessingG.html,
on background on Lessing, and Note 7, p.6 for his quotation.

- Nicholas Goodrick-Clarke,
Paracelsus: Essential Readings,
North Atlantic Books, Berkeley, Calif. (USA), p. 21, 30.

- Manly P. Hall,
Paracelsus:
His Mystical & Medical Philosophy,
Philosophical Research Society, 1997, p. 5; extracted from:
Fielding H. Garrison, A.B., M.D.,
An Introduction to the
History of Medicine - with medical chronology, suggestions
for study and bibliographic data, W.B. Saunders Company,
1929. p. 204.

- Ibid.

- Nicholas Goodrick-Clarke,
Paracelsus: Essential Readings,
North Atlantic Books, Berkeley, Calif. (USA), p. 19.

- I found no evidence that Paracelsus used a zinc chloride base
in his escharotics. It appears that ammonium chloride was
his halide caustic of choice in his own formulary work.
One prominent formula consisted of just three ingredients:
Orpiment (arsenic sulfide) -- good description:
http://mineral.galleries.com/minerals/sulfides/orpiment/orpiment.htm
Paracelsus' use of it in one cancer preparation:
Arthur Edward Waite, Alchemical Medicine - Paracelsus,
The Alchemical Press, Edmonds, Wash. (USA), p. 18.
He combined the orpiment with fuligo (wood soot), see
http://www.ibiblio.org/herbmed/eclectic/kings/carbo-lign.html
and with sal ammoniac (ammonium chloride) acting as the
caustic halide in this formula. One aside: Chloride and
iodine appear to be reoccurring halogens in this area,
as I have never seen any compounds of bromide, flouride,
let alone astatine, used in topical escharotic preparations.

- Paul Ehrlich (not to be confused with our celebrated ecologist
and author from Stanford) won the 1908 Nobel Prize in Medicine
for his work in immunity:
http://www.chemheritage.org/EducationalServices/
pharm/chemo/readings/ehrlich.htm
He is widely known for his REdiscovery an arsenic paste, his versions
called Salvorsan and Neosalvorsan was used in treating syphilis in the
early 20th century, and still in use in the veterinary community.
Ironically, he also coined the term "chemotherapy," a concept that was
synonymous with quackery at a time when x-ray and radiation treatment were
the prominent moneymakers in conventional cancer treatment. See:
Kenny Ausubel,
When Healing Becomes a Crime,
Healing Arts Press, Rochester, Vermont;
2000. p. 233; quoting:
Ralph W. Moss,
Questioning Chemotherapy, p. 15-16; A. Gilman
"The initial clinical trial of nitrogen mustard," American Journal
of Surgery, Vol. 105, 1963, pp. 574-78.

- As early as 1895, orthodox physicians were using arsenic paste
to treat skin cancer:
http://www.positivehealth.com/permit/Articles/Bodywork/rich16.htm

- Paracelsus used litharge (lead monoxide) in a topical paste for
cancer, which also contained salt water, alum (probably aluminum
sulfate), and white vinegar. Litharge is a strong enough irritant, though
not ideal by any means can be sufficiently transdermal to incure
other toxicological implications. See:
Arthur Edward Waite, Alchemical
Medicine - Paracelsus, p. 7. Also see:
http://www.jtbaker.com/msds/englishhtml/l3478.htm
MSDS Sheet for litharge (lead monoxide).

- Manly P. Hall
(1997), p. 7.

- Fielding H. Garrison, A.B., M.D.,
(1929), p. 205.

- Nicholas Goodrick-Clarke,
p. 19.

- A point made in the movie, When Healing Becomes a Crime,
by Ken Ausubel. See http://www.altcancer.net/vidgal.htm#hoxsey

- Jonathan L. Hartwell,
Plants Used Against Cancer,
Quarterman Publications, Inc., Lawrence, Mass.,
1982. This book is no longer in print, and when
I attempted in 1998 to get ahold of the publisher
at their address at 5 South Union Street in
Lawrence, Massachusetts (USA), the
current occupant said they had never even heard of
the publisher. Strange.

- http://www.altcancer.net/hartwell.com

- If you're a little weak in remembering your high school
chemistry, go to http://www.chemicalelements.com and
follow along. The halogens are the second to the last
column on the right, next to the noble gases. They
include (starting from lowest molecular weight to highest)
flourine, chlorine, bromine, iodine, and astatine.

- Nat Morris,
The Cancer Blackout,
Regent House, Los Angeles, Calif. (USA),
1977 (Fifth edition), p. 43. Dr. F.W. Forbes Ross (M.D.) treated
cancer as a mineral deficiency. He employed both potassium
iodine and potassium citrate (the latter NOT a halide) along
with phosphorus supplementation in London at the turn of the
nineteenth century. Says Nat Morris:
"In the treatment of cancer, Doctor Ross prescribed
potassium citrate and phosphate to correct the mineral
deficiency, with a weekly dose of five grains of potassium
iodide. His cancer patients were either the hopeless
and inoperable or those who had refused surgery
or irradiation. In a number of cases adjudged
as hopeless, he was remarkably successful. He pre-
scribed potassium routinely in all his other patients
and claimed that over a period of fifteen years no
patient under his care had contracted cancer."

- "Secret predates Mohs method: Perry Nichols and the
escharotic cancer cure." See:
http://www.dermatologytimes.com/dermatologytimes/
article/articleDetail.jsp?id=95680&pageID=1
Although this is an allopathic web site and the
article's author cannot faithfully report the facts
without lacing it with disparaging spin, the essential
points still come through.

- http://www.zompist.com/versci.htm

- The
Complete Pyramid Sourcebook, John DeSalvo, Ph.D.,
Great Pyramid of Giza Research Association, 2003.

- Ingrid Naiman,
Cancer Salves and Suppositories (1994), p. 41.

- Mohs, Frederic E., B.Sc., M.D., Chemosurgery:
Microscopically
Controlled Surgery for Skin Cancer. Charles C. Thomas Publisher,
Springfield, Illinois, 1978.

- Kenny Ausubel,
When Healing Becomes a Crime
(2000); p. 153-161. Hoxsey's Salve contained zinc chloride,
antimony trisulfide, and bloodroot. Note 29, p. 151.

- J.T. Phelan, H. Milgrom, H. Stoll, H. Traenkle. 1962. The use of Mohs'
chemosurgery technique in the management of superficial cancer
Surg. Gynec. Obstet. See: Harwell, p. 439, who notes "of 70
patients, 42 completely healed (of which 2 recurred)."

- An important side note: all three doctors originally
practiced in New York City, though both Fell and Pattison
ended up moving to London. This should appear to the
astute observer as more than coincidence.

- Nat Morris (1977), p. 30.
Most of the material on Blake, Fell,
and Pattison is this section is taken from Morris' work. The following
four footnotes are also Morris' and I provide them only on account
of the increasing unavailability of his fine work. The Cancer Blackout
was produced in five editions, the last of them having been printed
in 1977.

- Montague, M.F.A. and Musick, W.J.: A Yankee doctor in England
in 1859, Bull of the Hist. of Med., 13, 217-288, Feb., 1943

- Farrow, Ruth T.: Odyssey of an American cancer specialist,
Ibid., 23, 236-252, May, 1949.

- Nat Morris, p. 31.

 37b. J. W. Fell:
A Treatise on Cancer, London: John Churchill, 1857.
37b. J. W. Fell:
A Treatise on Cancer, London: John Churchill, 1857.

- Morris, p. 37.

- A. Hunton, "One some of the medical virtues of indigenous vegetables
grown in the United States. N.J. Med. Rep. found in Hartwell, p. 433,
wherein he notes, "(the ointment was) used successfully for over 30
years and obtained surreptitiously from an Indian doctor." (p. 432).

- Derrick Jensen,
The Culture of Make Believe, Chelsea Green
Publishing Company, White River Junction, Vermont (USA), 2004.
There are too many passages demanding thoughtful reflection
in this book, just on our treatment of the native American
Indians, to do it justice here. (And this is
only one of the themes of this, Jensen's last tomb). Among
the more noteworthy: p. 122 (destruction of heritage);
p. 162, 170 (General Sherman's treatment of them);
p. 172, 177, 308 (open Indian slaughter); p. 175 (Montezuma
slaughter); p. 193 (General Smith's "Burn and kill the
natives!" campaign -- "I want no prisoners. I wish you to kill
and burn; the more you kill and burn the better you will
please me" ... including children down to the age of ten);
p. 246 (the holocaust of the Cherokee indians); p. 311
(wipeout of Lakota and Cheyenne people), etc., etc. I had to
read this 608 page book twice while in prison. I was too busy
silently weeping to catch it all on the first go-around.
I underlined the parts that really struck a nerve on the
second pass -- which ended up being about 30% of the book.
Most people don't read footnotes -- and that's too bad --
I would have included this material in the main text
(more amplified, of course) if it were more germane to the
topic at hand. Actually, in a way, it is. You understand
in studying Jensen's work why a sustained medical holocaust
would not only be possible in our culture -- it is inevitable,
a mere reflection of its very sick, inner nature.

- Fell,
p. 95, noted in Hartwell,
p. 435. Fell himself was aware
that bloodroot ointment was made and used by Indians of the
Lake Superior region to treat cancer, even uterine.

- Treatment of cancer by bloodroot. 1859. Boston Med. and Surg. J.
noted by Hartwell, p. 437, wherein he notes the use of powdered
bloodroot to treatment cancers in Pennsylvania as early as 1811.

- J. Wolff, Die Lehre von der Krebskrankheit. G. Fischer Jena,
Part IIIb., 1914, p. 618. Noted in
Hartwell, p. 437, who comments:
"Folk remedy of the Indians of the Lake Superior region." (Breast
cancer). "Folk remedy in Russia (1896-1897)" for non-specific
cancers.

- National Cancer Institute, central files. Same citation for
members of the Larrea genus by Hartwell, p. 437, footnote #691.
His comments: "Cancer -- Louisiana; Pennsylvania; California;
Tennessee; (Cherokee Indians); Oklahoma. All 1956-7." Apparently,
Hartwell uses the same citation to communicate that the NCI was
well aware of its value as a salve and its common use in
Texas, with "1955-8" probably representing the dates during
which an internal investigation of its usage at NCI was made.

- Morris, p. 32.

- Ibid., p. 33.

- George Crile, Jr., M.D.,
Cancer And Common Sense,
Viking Press, New York, 1955. p. 31.

- Pattison, John:
Cancer: Its nature and successful and
comparatively painless treatment without the usual operation
with the knife, London: H. Turner & Co., 1866.

- Morris, p. 35.

- Ibid., p. 35.

- [ Find and cite Dr. Barbara's article in the June, 2000 issue
of the Journal of the American Medical Association. ]

- Morris, p. 38.

- Jonathan L. Hartwell,
Plants Used Against Cancer,
Quarterman Publications, Inc., Lawrence, Mass., 1982.
Section XI: Lloydia 34(4), p. 682.
It remains a mystery, even to this author, why despite
the depth of Hartwell's work, he only cites one reference
to any member of the Larrea genus (Zygophyllaceae Larrea tridentata).
Its use among the indians of the U.S. Southwest is extensive,
and yet he quotes a "Coville" source, noting "identified
from sample of leaves and twigs by Dr. B.G. Schubert, U.S.D.A."
Here is the reference Hartwell provides: "National Cancer Institute,
central files." For someone like myself who has worked
with indigenous sources for chapparal and knows how
ubiquitous its use was and is in the Southwest, this, in
and of itself, at least carries the appearance of a cover-up,
and this, coming from one of Hartwell's biggest fans.
Chapparal was too widely used for Hartwell to not have
been more familiar with its indigenous use in the
treatment of cancer.

- Alma R. Hutchens,
Indian Herbology of North America,
Shambhala Publications, Inc., Boston, Mass, 1973. p. 82-84.
The Indian nations of Papoga, Pimas, and Maricopas,
among others, were users of the Larrea genus
to treat a variety of ailments including arthritis,
cancer, chronic backache, acne and other skin
ailments, including skin cancer; kidney infection,
leukemia, bronchial and pulmonary conditions, etc.
- Anthony J. Chichoke, D.C., Ph.D.,
Secrets of
Native American Herbal Remedies, A Comprehensive
Guide to the Native American Tradition of Using
Herbs and the Mind/Body/Spirit Connection for
Improving Health and Well-Being, Avery (Penguin
Putnam, Inc.), New York, 2001. p. 35.
- Judith Sumner,
The Natural History of Medicinal
Plants, Timber Press, Inc., Portland, Oregon;
2000, p. 172, 213. Notes the historic use of Larrea to
treat skin infections, but falls for the fallacious
orthodox admonition about "acute" hepatotoxicity. Shame.
- Morris, p. 27-29.

-
 I have collected just seven of the Sanatorium's "annual yearbooks"
over the year's, the majority of each volume consisting of the name, home state, cancer type,
and personal address of each cured patient -- something you would never see today.
In just the few volumes I own, there are thousands of cases, some of those who have been
described to me my relatives are nothing short of miraculous.
I have collected just seven of the Sanatorium's "annual yearbooks"
over the year's, the majority of each volume consisting of the name, home state, cancer type,
and personal address of each cured patient -- something you would never see today.
In just the few volumes I own, there are thousands of cases, some of those who have been
described to me my relatives are nothing short of miraculous.

- Williams, p. 1463-1464.

- Ibid.

- Additionally, Dr. Nichols died following an operation.
Though he succeeding in the budding world of alternative practice,
the conventional procedure contributed to his undoing. See
Perry Nichols Death Certificate,
also see his locally published obituary.

- See Savannah Reporter, Apr. 29, 1976.
Also Nichols Perry appears to have drafted an informal will on the Sanatorium's letterhead,
clearly indicating his intentions : pg.
one,
two, and
three. Although the document does not appear
to have been signed, it reflects that actual turn of events that followed his passing.

- See : Savannah Reporter, Jan. 18, 1929.
Comment about the success of the 1929 business year to be found at
Savannah Reporter, Nov. 29, 1929.
 . .
- See: Savannah Reporter, July 5, 1942,
followed by pages two
and three.
 . .
- I've converted the article, also taken from Whale.to,
into an easy-to-read Word file.
Dyer did a more detailed article
two years
later (Clinics in Dermatology (2006) 24, 458-460.
 . .
- Ibid.
- Ibid.
- The New Encyclopaedia Britannica, 15th Edition, 1986,
Vol. 3 (Micropaedia), "Celsus, Aulus Cornelius," p. 16.

- Ibid.

- Ibid.

- Ingrid Naiman,
Cancer Salves and Suppositories,
Seventh Ray Press, Cundiyo, New Mexico (USA); 1994, p. 72.

- Ibid., p. 94.

- Ibid., p. 100.

- See http://www.cancersalves.com/introduction/zncl.html.

|
Recent Addition (2017):
 The Truth?
The Truth?
It Cures Cancer.
99% of The Time
Topically. Period.
 Granted, skin cancers are the
easiest to treat and cure. But the scandal behind escharotics is
that this skin cancer cure has existed for literally hundreds of
years -- something you learn by the time you complete Chapter 2
to the left. The zinc chloride-based "modern escharotics" have
been in regular use since the 1850's, though always the target
of suppression by the orthodox medical community.
 The reason for this
suppression is obvious: skin cancers represent a large
percentage of the dermatologist's business. In some areas,
basal and squamous cell carcinomas and melanomas and
their pre-cancerous keratotic cousins represent better
than 50% of their work. The AMA and pharmaceutical
companies work very hard to maximize their market share.
Anything that works this well, this inexpensively, and
has self-diagnostic properties so that you don't need
the assistance of a physician, makes it anathema.
Blackout
... it's hard
to determine which is more nauseating: the horrid stories of
suppression and abuse in the cancer industry that
Morris' revealed in 1959 ... or that nothing has
changed in the over 45 years since. For more
information on Suppression in the Cancer
Industry and a list of suggested reading,
see the page,
Cancerolytic
Herbs: A History of Suppression -- on the
Alpha Omega Labs site.
Treatise on Cancer
 J. Weldon Fell, published his
"Treatise on Cancer and Its Treatment" in 1857. An American with an
extraordinary success at curing cancer in his practice in New York,
he became an "ex-pat" in London to escape droves of jealous
colleagues in the States. Although the book is just 95 pages,
the last 30 pages are devoted to some of Dr. Fell's more
astonishing cures. Instead of including melanomas or other
easier cases (which is child's play to cure for those who
know how to work with escharotics), he includes those instances
which were considered among the toughest type cancers to cure in
his day. The predominant number of cases he reports in the book
are, therefore, breast cancer cases. Other cases he reports
include one uterine and a couple of epithelial cancer cases
of the nose --
similar to those which comprise the "Sue Gilliatt" type
frivolous lawsuits of the 21st century.
Cancer Salves
 Naiman also provides her own
"history of escharotics," some of which is incorporated into the text
at left. However, the practicum material is so inaccurate it makes
me wince at times. She states in one place
that " ... starting from the beginning, it should
be underscored that the experts, from Hildegard
to the present, have all more or less concurred
that the salves are not a cure. At best, they
are an alternative to surgery. There is nothing
about them that would prevent recurrence."
[ 71].
Well, that just isn't true.
 An experienced
user of escharotics knows that to be mind-numbingly
preposterous. Or perhaps Ms. Naiman wasn't working
with some of the better formulas. Cansema, for one,
is a cure. And non-reoccurence is the rule.
Frankly, in the thirteen years that I made and sold Cansema,
I would say that AT LEAST 50% of all users saw
absolutely no recurrence in their skin cancers,
or other growths removed near the skin. At least.
I myself have used Cansema on about five growths
over the years. Only one of them returned
such that I had to do another application, and
that was about eight years later. Now, I realize
that some of this may be attributable to the Cansema
formula itself, refined as it was through constant
reappraisal of end user and health care practitioner
inputs over a thirteen year period.
 In another
place Naiman says, "even the most fervent advocates
of the salve do not recommend the salves as a
substitute for proper diagnoses."
[ 72. What she doesn't
tell you is that this recommendation is made to
mollify the all-powerful medical lobby. No
experienced escharotic practitioner believes
that their product is not self-diagnosing
(i.e. it reacts only to cancerous or precancerous
tissue). If an escharotic formula does NOT react
to only cancerous or precancerous tissue than it
is an inferior formula. So someone would make
Naiman's statement only if they were inexperienced
in the actual use of escharotics from a clinical
point of view, or they dealt in inferior formulations,
or they were cowtowing to the medical lobby to cover
their hide. I can now speak honestly about this matter
because I no longer make or sell my
formulas. Prior to my incarceration, I had to lie
just like everybody else.
 And do
heal
overs really take as long as "seven months"?
Naiman says this is "not unusual."
73.
Such an occurrence was very rare with
Cansema.
 On her
web site,
Naiman made the statement:
"I do not think zinc chloride has much capacity to discriminate healthy from malignant tissues. Depending on scar tissue and pigmentation and some other variables, it might be more readily absorbed by certain tumors, but the healthy tissue is definitely not impervious to this product.
 "Zinc
chloride is made by pouring hydrochloric acid over zinc. It is extremely caustic and will not merely damage skin but result in possibly extreme pain and scarring. However, it can be washed off with water when accidental contact is made outside the intended treatment area. Just keep in mind that it is caustic and needs to be used sanely and carefully." "Zinc
chloride is made by pouring hydrochloric acid over zinc. It is extremely caustic and will not merely damage skin but result in possibly extreme pain and scarring. However, it can be washed off with water when accidental contact is made outside the intended treatment area. Just keep in mind that it is caustic and needs to be used sanely and carefully."
 Quite recently, she deleted the information
on this one page and archived it, but then the very same information
appears on her
"zinc
chloride and bloodroot" page
( 74). To counter this inaccurate
information I added an FAQ
question to the Alpha Omega Labs' site, plus a picture
of my own hand scooping up a handful of zinc chloride,
which I have worked in for up to an hour at a time with
only mild skin irritation. (See picture below).
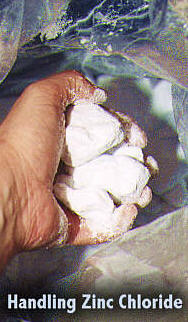
 This is a sensitive issue
for those of us who have worked with escharotics, because
it is a standard piece of disinformation that the medical
establishment espouses to scare people away from
escharotics. After all -- why would anybody want to use
a product that destroyed healthy as well as cancerous
tissue? ... (though, quite ironically, conventional
chemotherapy destroys both healthy and cancerous cells).
 Its a malicious
lie with no basis in scientific fact. Zinc chloride has
a pH of about 5.0 and is only mildly caustic.

Harry Hoxsey
 Kenny Ausubel is to Dr. Harry
Hoxsey what Barry Lynes is to Dr. R.R. Rife.
Both biographers brought their subjects to
the attention of the world.
 Ausubel went
the extra step and had a movie made,
which can
still be viewed
on the Alpha Omega Labs web site.
 The relevance
of Hoxsey's work to this chapter is the degree to
which money and politics suppress even the most
effective medical treatment that does not curry
favor with the orthodox medical establishment, which
demands that cancer treatment, in particular,
meets the standards of their "high profit paradigm."
Most effective cancer treatments are very inexpensive,
and that makes them worthy of suppression. You get
extreme doses of this reality when you study
Hoxsey -- the success of his clinics and the
tens of thousands who came to his support
when the FDA came after him. The story of
Hoxsey is the story of the brutality of profits
over humanity, decency, and scientific principle.
 The Hoxsey story
has become a fitting metaphor for what's wrong with
the "disease care" system we have today that has
turned the health needs of ordinary citizens into a cruel
system of financial servitude.

Rx Business
 We cover some of this
same territory with Wohl's 1984 work,
The Medical
Industrial Complex. Written in 1958, one gets a sense
that the problem goes back to antiquity -- that organized
medicine is inherently dangerous to one's health and
callous to the needs of the ordinary person. He opens
with a quote from Hippocrates (circa 400 B.C.) that is
as true today as it was nearly 2,500 years when written:
"Although the art of healing is the most noble
of all the arts, yet, because of the ignorance
both of its professors and of their rash
critics, it has at this time fallen into the
least repute of them all. The chief cause
for this seems to me to be that it is the only
science for which states have laid down no
penalty for malpractice. Ill-repute is the
only punishment."
 In light of
a 500 year suppression of escharotic preparations,
one gets the sense that the "politics and greed"
have been there all along. It's gotten worse,
to be sure, but the seed was there long ago.

Treating
The Insane
Insanely
 Your initial
impulse might be one searching for relevancy.
What does our treatment of the insane have to
do with the suppression of medical technology
to feed a hungry profit-driven vortex of
corporate greed?
 Everything.
 The way we
treat those in our midst who are LEAST predisposed
to speak for, represent, or defend themselves speaks
volumes about how everyone else gets treated.
Sanity is, after all, an entirely relative thing.
 Whitaker's
title truncates the essence of things, "Mad in
America: Bad Science, Bad Medicine, and the
Enduring Mistreatment of the Mentally Ill" (2001).
The work itself is paced in four parts,
dividing the American approach to the
mentally ill into "The Original Bedlam"
(1750-1990); "The Darkest Era" (1900-1950);
"Back to Bedlam" (1950-1990s); and
"Mad Medicine Today" (1990s - Present).
 The truth is
not only shocking, but reflective of the fertile
soil in which one would expect the suppression of inexpensive,
highly effective medical technologies to flourish.
Amazingly, schizophrenics in the U.S. fare
worse than patients in the world's poorest
countries, "and quite possibly worse than
asylum patients did in the early 19th century ...
as a society (we are) deeply deluded about
their efficacy."
 Whitaker
traces a history of treatment specifically designed
to "silence patients and dull their minds."
(Parallels?) Early on, patients were routinely
"spun" until they grew "so weak and dizzy they
couldn't move." They had their teeth, ovaries,
and intestines removed, and in one shocking
therapeutic contribution that speaks volumes about the inhumanity
in orthodox medicine, patients were submerged in
water so cold that hypothermia resulted.
 When eugenics
became the rage in the 1920's and 30's, other even
more horrific therapies were introduced. The
"lobotomy" was introduced that "worked" by damaging
the brain, followed in the 1950's by electroshock
and wave after wave of news that did little more
than impair the patient. Neuroleptics numbed
the nervous system and restricted motor movement.
As studies emerged showing that these drugs didn't
work, they were pushed aside under the influence
of the powerful drug companies who made them.
A litany of examples in the book show how the
drug companies skew their studies and "employ
charlatan scientists" to run them. The fact is,
the new, more expensive "atypical" drugs are no
more effective than the old; only, a new set
of side effects have been found. Even more
disturbing, patients have been encouraged to
participate in experiments that
"exacerbate their delusions." The money motive
of the drug companies has a strong flavor that
saturates the last two "parts" of the book.
 And that brings us
to my reason for including it as the final literary
example for this section on medical suppression.
 In another era,
another age ... another place in time, the physician
took a Hippocratic Oath to "do no harm..." and ...
he meant it. In another era, another age,
curing the patient was primary; making money
was secondary. Are we, too, not patients?
Are we, too, not being "dumbed down,"
anesthetized to the primary motives that drive our
so-called "health care system"? Are we not treated
in the same way that the insane are treated,
the renderings just not as obvious? Are not all
the same elements of cruelty, brutality, and
callous disregard still left intact? One cannot
study the history of the suppression of simple,
effective, medical approaches, and then read this
book without seeing the obvious correlations.
 We may
respond to a different poison, but we drink from
the same cup.
 Note: Note: The
photos below are thumbnails. Click on each to see enlargements.

 In 1905 Nichols was asked to head an
80-bed sanitorium in Hot Springs, South Dakota. It would be his last major
move before settling down in Savannah, MO.

 A review of the extent documentation left behind
by Dr. Perry Nichols reveals an obsession with the retaining of personnel who were both
technically competent and morally upright. On this basis alone, Nichols' cleaving the
more objectionable elements of industrial medicine becomes apparent. The photo above
shows Dr. Nichols, along with leading members of his administration.

 Throughout the life of the Sanatorium in Savannah,
the organization was prolific in its production of printed materials for the general public:
yearbooks, magazines, postcards, etc. The common theme in this entire effort was the attempt
to let the world know that the cure for cancer was simple, safe, and minimally invasive in the
vast majority of cases. And the evidence they provided to make their point was nothing
less than breathtaking.

 Sanatorium foyer.

 Sanatorium dining room for patients.

 To accommodate the 200-bed Sanatorium with its very low
vacancy rate, the kitchen had to be a small industrial kitchen.

 Office at the Sanatorium.





 Five Photos Above: Five Photos Above: Images of the
patient room accommodations.

 A leisurely moment outside the Sanatorium with members of the staff.

 The Sanatorium made a number of modifications / expansions
over the years. Above, nurses on the staff participate in a light-hearted mock photo op.

 A group shot with Sanatorium patients.


 Nurses on staff.

 The Nichols Sanatorium was an enormous boon to the local
economy, filling hotels with visiting patient visitors, relatives, well-wishers, and others who
would not otherwise stay at the Sanatorium itself.

 View of the side entrance to the Sanatorium. The guard shack
is in the foreground, "Building #2" behind it and to the right, and the edge of the main building of the Sanatorium
is shown on the far left.

 View of Building #2.

 View of Building #2 during construction, built to
accommodate the Sanatorium's expansion.

 Dr. Nichols must have known, when he wrote an informal "Will"
for his staff, that the Sanatorium would long outlive him. In fact, he wrote this "Will" in 1924,
a year before his death. The excerpt above was reprinted in a subsequent
issue of the Sanatorium's magazine and it sums up the mission statement of the institution:
"You have all known me long and well. It is my will and desire that the management of the Sanatorium
and my business generally be continued as nearly as possible on the lines and methods now being used
in the management of said hospital and business. The changes in business methods that time may bring,
as well as any and all other changes in the present program, should be viewed with the closest scrutiny,
it having long been proven that changes in our present plans and system have been damaging; that our present
methods have long been standing, long been tested out and while some changes will, from time to time,
become necessary, these should be made under the greatest precaution. I would not endeavor to convert this
business into a purely money-making institution; I would endeavor to make others happy to the extent of the
greatest numbers possible for me to do, never striking down unless morally sure immensely greater good
can be derived therefrom. I am trusting to the executives and members of this corporation to take into account
the substance of this letter. ~~~ Perry Nichols
|





































